How Do You Get Pregnant Naturally
[ Source : American Pregnancy Association ]
You may be asking this question because you want to know how pregnancy happens, but more than likely you are wanting to know how to conceive naturally. You are probably looking for the quickest and easiest way to get pregnant without interventions. You may be interested in getting pregnant naturally because of philosophical or religious reasons, health concerns, or just because you prefer not to use interventions.
Physical Health
The first thing you can do to get pregnant and to have a healthy pregnancy is to be physically healthy. It is important to not be over or under weight, both of which have negative effects on fertility and healthy pregnancies.
You also want to make sure you are exercising 3 to 4 times a week. Aerobic exercise is essential because it helps blood circulation and improves lung capacity. Incorporating weight-bearing exercises helps you gain muscle strength and lose weight easier, while yoga exercises help you work on posture and balance. This all contributes to a healthier you, which increase your chances of conception and a healthy pregnancy.
Physical health starts with how you treat your body. While exercising during pregnancy is an essential step towards a healthy you, it is more important you are not doing anything counter-productive for fertility and a healthy pregnancy. It is imperative you remove any unhealthy habits or practices that limit or decrease your physical health.
For maximum health you should eliminate or reduce the following:
Smoking
Alcohol
Recreational Drugs
Hazardous Chemicals
Caffeine
You may also want to talk to your healthcare provider regarding any prescription medication you are taking. Some medications are harmful to take during pregnancy. It is possible that your provider may want to forego or alter the medications you are taking to help increase your chances of conception and having a healthy pregnancy.
Additionally, eating healthy, well-balanced meals, along with ensuring daily consumption of certain nutrients and vitamins, is directly related to your health and wellness. Check out our article on preconception nutrition and health for men and women for other helpful ideas. Your Ovulation When Trying to Get Pregnant Naturally
Ovulation
One of the keys to easy conception is knowing when ovulation is occurring. You can track ovulation with a fertility monitor or ovulation predictor kits. However, you can track your and predict your ovulation naturally without using these types of kits.
If you have a regular cycle that occurs every 28 to 32 days, you should be able to track your ovulation using the calendar method. This is simply recording the first day of your last menstrual period on the calendar and finding the corresponding next menstrual period day. Once you have that, you can count back 8 to 18 days and know that ovulation will occur on one of those days. With an average 28 day cycle, ovulation will occur on one day between the 11th and 21st cycle days (29 day cycle, 12-22 days; 30 day cycle, 13-23 days; and so on).
A second way to track ovulation is through monitoring the changes in your cervical mucus. As you get closer to ovulation, your mucus will become wetter, more slippery, and stretchier. It is often compared to egg whites. Ovulation is directly related to this change, and the day that you notice the most of this egg white discharge is the day you are expected to ovulate.
You can also use a basal thermometer to track your basal body temperature. Your basal body temperature will spike right after ovulation.
These techniques for tracking your ovulation naturally are part of a family planning method called fertility awareness or natural family planning (NFP). You can learn more about the calendar method, cervical mucus, and basal body temperatures in the article, Fertility Awareness. Get Pregnant Naturally
Timing Intercourse
Some people try to time sex so that it is during or right before ovulation. While this can work, there is a better approach to your sex schedule for those trying to conceive. If you have a regular cycle occurring every 28 to 32 days, then you should be able to leverage a typical fertility window for planning sex.
For the above mentioned regular cycles, you should know ovulation typically occurs between day 11 and day 21 of your cycle. What most people don’t know is sperm can live inside you from 2 to 5 days following intercourse. You can use our free Ovulation Calendar to help identify your fertility window.
The best chances for conception occur if the sperm (semen) is already inside waiting for the egg to be released. To maximize your efforts to try to conceive based on this information, here is how to approach your sex schedule and increase your efforts to conceive.
Count out 10 days from the first day of your last menstrual period. Have sex this day and then every other day, for the next 10 days. Having sex every other day helps ensure you have healthy mature sperm delivered with each intercourse. This schedule will place semen inside waiting for the egg to be released, while also adding sperm during ovulation.
Nutrition
Nutrition is directly related to your physical health. However, nutrition is also tied to conception and healthy pregnancies. It is essential to eat well-balanced meals full of the recommended nutrients and vitamins that are tied to your health and wellness. Combined with exercise, this is one of the most important steps for a healthy you, and which is directly related to your fertility health.
You should be looking to the appropriate daily intake of carbohydrates, fiber, protein, and essential fats. Apart from healthy eating, there are some key nutrients that are tied to your fertility wellness and make it easier to get pregnant naturally.
Folic Acid : Folic acid is tied more to healthy fetal development than conception, but because this vitamin is so essential during the first few weeks of pregnancy, it is important to highlight it now. Make sure you are getting 400 to 800 mcg of folic acid a day, as this helps to prevent neural tube defects.
Nutrients, Vitamins, and Nutritional Facets
Here is a list of some the key nutrients, vitamins, and nutritional facets you need to make sure you are part of your diet regularly:
Water – Drinking water helps support organ function, supports hormonal balance, and helps carry out toxins from the body. Collectively, this helps support your fertility.
Complex Carbohydrates – Eating vegetables, whole grains, and fruits help you get nutrients that support your fertility and provides fiber that works with water to help remove toxins from your body.
Protein – Eating protein supports your fertility by providing nutrients that contribute towards hormone production. However, red meat should be lean and limited. High red meat diets can lead to problems with endometriosis.
Fatty Acids – Eating oily fish like mackerel and salmon, along with nuts and seeds, is a great way to get fatty acids that support your fertility and the development of your baby once you conceive.
Whole Milk – Drinking whole milk is related to your fertility. A study by Chavarro and Rosner found that women who drank 3 or more glasses of whole milk a day were 70% less likely to be infertile due to failed ovulation.
Zinc – Zinc deficiencies have negative effects on fertility for both men and women. Taking 15 mg of zinc daily help both men and women enhance their fertility. Zinc can be found in vegetables, eggs, whole grains, peas, onions, beans and more.
Vitamin B6 – Getting this vitamin daily helps in your production of the female sex hormone while also supporting the regulation of estrogen and progesterone. Vitamin B6 is found in eggs, salmon, peanuts, bananas, and soy beans.
Vitamin C – Vitamin C helps trigger ovulation for women and supports healthy sperm count and mobility for men. Vegetables and fruits like strawberries, oranges, and blueberries all contain Vitamin C.
Vitamin E – Men and women both benefit from Vitamin E consumption. This vitamin affects hormone function for women and enhances sperm quality for men.
Foods to Avoid When Trying Get Pregnant Naturally
Eating healthy directly supports your health and wellness while eating poorly reduces your health and wellness. To maximize your health and wellness and ultimately your fertility wellness, there are nutritional items you should avoid to increase your chances of getting pregnant naturally.
Here is a list of things to avoid or at least limit your consumption:
Caffeine – Caffeine reduces calcium absorption, and some research shows that it lowers your fertility by approximately 27%.
Processed Foods – These contain pesticides, artificial hormones, and preservatives, which collectively have a negative impact on your health and wellness.
Red Meat – High consumption of red meat can lead to endometriosis, which can negatively affect your efforts to conceive.
Soy Products – Soy consumption by men has been connected to lower sperm counts.
Important Points in the Differentiation of Gynecological Disorders
The Key signs and symptoms in diagnosing are those relating to menstruation, leucorrhoea, pregnancy and labor. Systemic signs and symptoms are secondary in importance and should be disregarded if they conflict with the key symptoms.
Deficiency-Type Patterns
Qi Deficiency
Clinical manifestations include a shortened menstrual cycle with profuse thin, pinkish flow, uterine bleeding, uterine prolapse, persistent pale lochia following childbirth and spontaneous secretion of milk after delivery.
Blood Deficiency
Clinical manifestations include a prolonged menstrual cycle with scanty thin, pinkish flow, amenorrhoea, post menstrual abdominal pain, miscarriage and insufficient lactation.
Spleen Deficiency
Clinical manifestations include persistent uterine bleeding, a profuse thin, odorless, white vaginal discharge, pernicious vomiting and oedema during pregnancy.
Kidney Deficiency
The manifestation of Kidney Yin Deficiency include a scanty red or dark menstrual flow, irregular menstruation, uterine bleeding, amenorrhea, miscarriage and eclampsia or threatened eclampsia.
The manifestation of Kidney Yang Deficiency include a thin, pinkish menstrual flow, irregular menstruation, uterine bleeding, a profuse thin vaginal discharge and infertility or miscarriage.
Excess-Type Patterns
Qi Stagnation
Clinical manifestations include an irregular menstrual cycle, hesitant and painful menstrual menstruation, pelvic inflammation, pernicious vomiting, palpable abdominal masses and retarded secretion milk.
Blood Stagnation
Clinical manifestations include a prolonged menstrual cycle, dysmenorrhoea, uterine bleeding, amenorrhea, pelvic inflammation, palpable abdominal masses, persistent purple lochia with clots and boring abdominal pain which is aggravated by pressure.
Phlegm-Damp
Clinical manifestations include a profuse vaginal discharge, amenorrhoea, infertility, pernicious vomiting and oedema during pregnancy.
Heat Patterns
Excess-type Heat Patterns
Clinical manifestations include a shortened menstrual cycle with profuse deep-red flow, epistaxis during menstruation, uterine bleeding, vaginal bleeding during pregnancy and thick, deep-yellow leucorrhoea.
Deficiency -type Heat Patterns
Clinical manifestations include a shortened menstrual cycle with bright-red flow, or a prolonged dribbling flow, hypertension during pregnancy and threatened eclampsia.
Cold Patterns
Deficiency-type Cold patterns
Clinical manifestations include a prolonged menstrual cycle with scanty pinkish flow, dysmenorrhoea, amenorrhoea, a watery vaginal discharge, pernicious vomiting, infertility, palpable abdominal masses and lingering abdominal pain which is alleviated by warmth and pressure.
Excess -type Cold Patterns
Clinical manifestations include a prolonged menstrual cycle with scanty dark-red flow, infertility, palpable abdominal masses, dysmenorrhoea, amenorrhoea and abdominal colic which is alleviated by warmth.
Natural Pregnant
IUI
(Intrauterine insemination)
IVF
(In-Vitro Fertilization)
Fertility Support
ADVANCED
RedAcu.Com
Promoting Self-Healing
" There is nothing to compare with your health. "
25222 Grogan's Mill Road, The Woodlands, Texas 77380
www.RedAcu.com
Dr.Kim's Unique techniques and Approaches
Before pregnancy - Unexplained infertility, Low Ovarian Reserve, . . . .
Recurrent miscarriage, Unexplained miscarriage, . . . .
During Pregnancy - Morning Sickness, Pain, Autoimmune disorders, ...
Before due date - Breech presentation, Premature contractions,
Post-partum recovery and other
Post-partum depression, ....
How does inflammation affect pregnancy ?
Study confirms that inflammation during pregnancy is linked to baby's brain. Inflammation is a normal part of the body's response to infection, chronic stress or obesity. In pregnant women, it is believed that heightened inflammation increases the risk of mental illness or brain development problems in children.
Can inflammation cause a miscarriage ?
Most relevant studies in animals and humans indicate that some degree of systemic or uterine inflammation is necessary both for normal implantation and pregnancy. However, if inflammation becomes too excessive it might cause pregnancy complications such as fetal resorption/miscarriage.
What are some common autoimmune disorders that can cause a miscarriage?
Systemic Lupus.
Crohn's Disease.
Rheumatoid Arthritis.
Scleroderma.
Addison's disease.
Celiac disease.
Can inflammation in the uterus cause infertility ?
Inflammation has a significant role in gynecology and infertility, affecting the ovary, uterus as well as the embryo and implantation.
Does inflammation affect fertility?
Inflammation is your body's natural response to injury or illness. However, prolonged inflammation can lead to insulin resistance and studies suggest it is linked to many conditions that may affect fertility, such as endometriosis, PCOS, implantation failure and recurrent miscarriage
What can cause miscarriage after 8 weeks?
Other causes of early miscarriages at 6 weeks to 8 weeks
Anatomical abnormalities of the uterus. Uterine malformations can cause recurrent miscarriages if they remain undetected. ...
Infections. ...
Uncontrolled diabetes or high blood pressure. ...
Thyroid disease. ...
Blood clotting. ...
Medications. ...
Food poisoning. ...
Environmental causes.
Why do I keep having miscarriages at 6 weeks?
An unbalanced translocation then can become cause for even repeated miscarriages. Miscarriages can also be caused by anatomical abnormalities of the uterus, such as uterine septa or fibroid tumors (myomas) or even small endometrial polyps.
Why do I keep miscarrying at 7 weeks?
Recurrent early miscarriages (within the first trimester) are most commonly due to genetic or chromosomal problems of the embryo, with 50-80% of spontaneous losses having abnormal chromosomal number. Structural problems of the uterus can also play a role in early miscarriage.
What is the most common chromosomal abnormality in miscarriage?
The most common chromosomal abnormality is Trisomy 16 which occurs in 26% of losses. Trisomy 16 is incompatible with life and has never been described progressing more than 11 weeks of gestation.
Are all miscarriages due to chromosomal abnormalities?
About 80% of all pregnancy losses occur within the first trimester and are often caused by having missing or extra chromosomes, called aneuploidy. Sporadic errors during chromosomal division and duplication cause aneuploidy. Many of the abnormal chromosomes are incompatible with life and result in miscarriage.
Can sperm cause chromosomal abnormalities?
Because half of a developing baby's chromosomes come from the father, it is possible that he may contribute abnormal chromosomes to a pregnancy. About three out of four miscarriages occur during the first trimester of pregnancy.
Does sperm quality affect baby?
Clearly, having healthy sperm is important. But sperm health goes beyond just conceiving. Sperm quality also plays a role in the health of the overall pregnancy and possibly the baby. In studies on mice, stress and obesity in male mice modified the genes carried in their sperm
Can a father's sperm cause miscarriage?
The quality of a man's semen also seems to play a role. “Poor sperm quality can be the cause [of miscarriage] in about 6% of couples,” says Dr. Gavin Sacks, an obstetrician and researcher with IVF Australia. But there are probably multiple factors that, together, result in a lost pregnancy, he adds.
Can stress cause birth defects?
Stress results in increased catecholamine production, which in turn leads to decreased uterine blood flow and increased fetal hypoxia. Animal studies indicate that hypoxia affects a variety of developmental processes (eg, cell death)29 and organ systems, which could result in various types of birth defects.
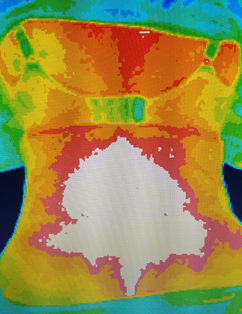
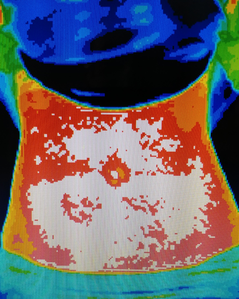
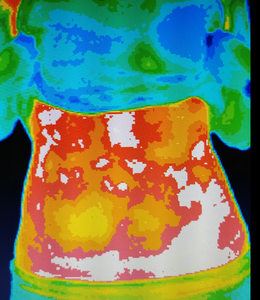
Inflammation affects your pregnancy !!!
Inflammation level (heat) : White color > Red > Orange > Yellow > Green > .........